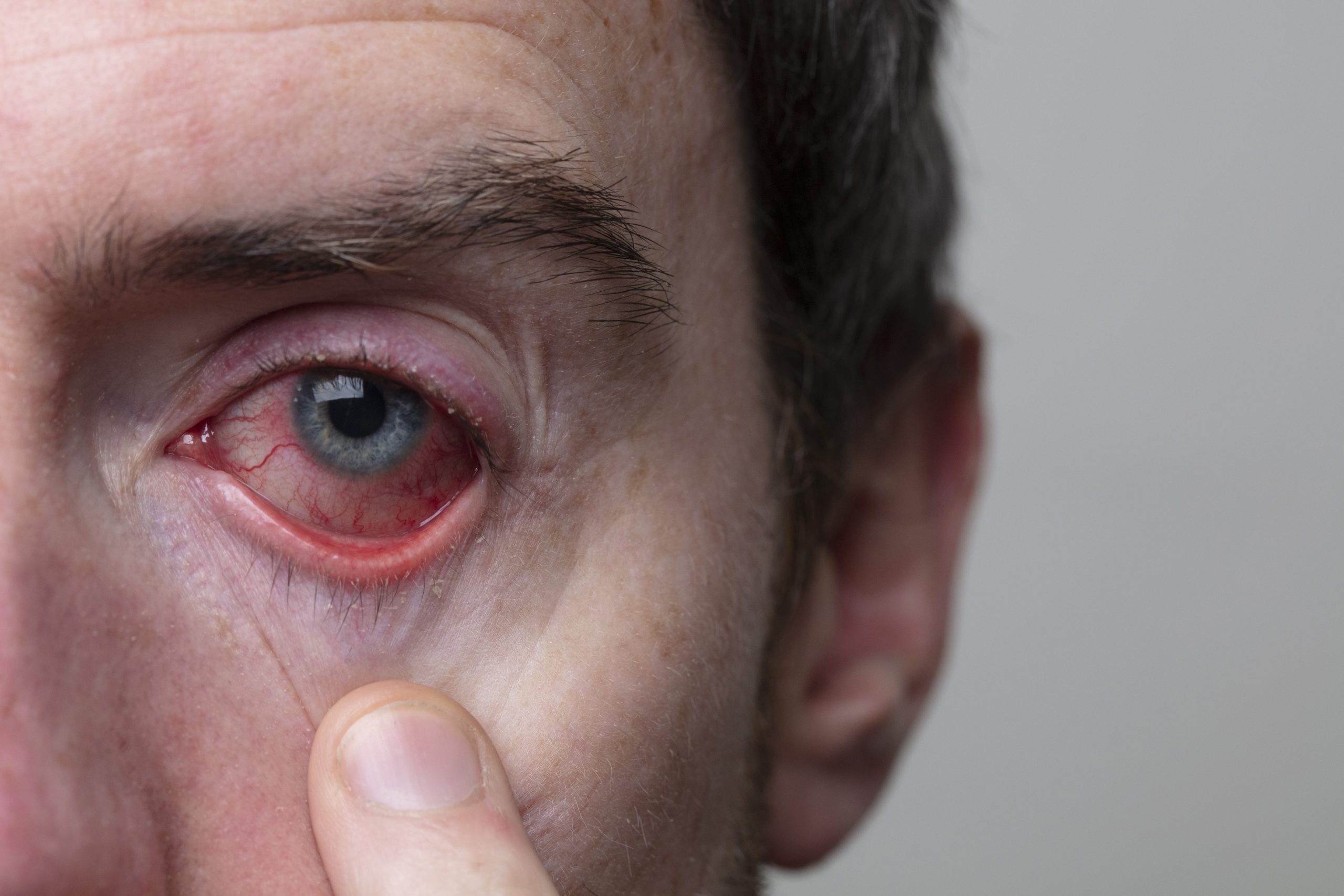
Are your eyes red, painful, and causing blurred vision? You might be dealing with uveitis, an inflammation in the middle layer of your eye. If left untreated, it can lead to permanent vision loss or even blindness. With about 30,000 Americans losing their eyesight every year due to uveitis, it’s crucial to seek medical attention promptly. In this article, we’ll discuss the causes, symptoms, and treatment options for uveitis, along with tips for prevention and living with this condition.
Uveitis Symptoms
If you’re experiencing redness or pain in your eyes, along with sensitivity to light and blurry or decreased vision, it may be a sign of uveitis. These symptoms can occur suddenly and worsen quickly, or develop gradually over time. It’s important to seek medical attention if you’re experiencing these symptoms to prevent any potential vision loss.
Eye redness
Eye redness is a common symptom of uveitis, indicating inflammation within the eye. Uveitis is a condition in which the uvea, the middle layer of the eye, becomes inflamed. This inflammation can affect various parts of the eye, including the anterior chamber. The exact cause of uveitis is often unknown, but it can be associated with autoimmune or inflammatory disorders, infections, medication side effects, eye injury or surgery, and rarely, eye cancer. Eye redness in uveitis is a result of the inflammation and increased blood flow to the affected area. It is important to seek medical attention if you experience eye redness, as untreated uveitis can lead to vision loss.
Eye pain
As you continue to explore the symptoms of uveitis, let’s delve into the experience of eye pain that can accompany this condition. Eye pain is a common symptom of uveitis and can range from mild discomfort to severe and debilitating pain. The location and intensity of the pain may vary depending on the type and severity of uveitis. To give you a better understanding, here is a table summarizing the different types of uveitis and the associated eye pain:
| Type of Uveitis | Location of Eye Pain | Intensity of Eye Pain |
|---|---|---|
| Anterior uveitis | Front of the eye | Mild to moderate |
| Intermediate uveitis | Around the eye | Mild to moderate |
| Posterior uveitis | Back of the eye | Mild to severe |
| Panuveitis | Throughout the eye | Severe |
If you are experiencing eye pain along with other symptoms of uveitis, it is important to seek medical attention for proper diagnosis and treatment.
Light sensitivity
When experiencing uveitis, a common symptom that may accompany eye pain is sensitivity to light. This sensitivity, also known as photophobia, occurs when your eyes become overly sensitive to bright light, causing discomfort or pain. You may find it difficult to keep your eyes open in bright environments, and even normal lighting may feel too intense. Light sensitivity is a result of the inflammation in the eye caused by uveitis. The severity of light sensitivity can vary from person to person and may depend on the type and severity of uveitis. It is important to protect your eyes from excessive light exposure by wearing sunglasses or avoiding bright lights when you have uveitis.
Blurred vision
If you have uveitis, one of the common symptoms you may experience is blurry vision. This occurs because the inflammation in your eye can affect the clarity of your vision. Here are four things you should know about blurry vision and uveitis:
- Blurry vision can vary in severity, ranging from slightly blurred to significantly impaired vision.
- The blurriness can affect one or both eyes, depending on the type and extent of uveitis.
- It may be accompanied by other symptoms such as eye pain, redness, and sensitivity to light.
- If you notice blurry vision or any other changes in your vision, it is important to seek medical attention promptly to determine the underlying cause and receive appropriate treatment.
Decreased vision
If you have uveitis, one of the symptoms you may experience is decreased vision, which can be a result of the inflammation affecting the clarity of your vision. Uveitis is inflammation inside the eye that can damage the uvea, the middle layer of the eye. The uvea consists of the iris, ciliary body, and choroid. The inflammation can affect one or both eyes and if left untreated, uveitis can lead to vision loss. The decreased vision can occur suddenly, worsen quickly, or develop gradually. It is important to seek medical attention if you notice any changes in your vision or other symptoms associated with uveitis. Prompt treatment can help minimize long-term vision problems and preserve your eyesight.
Uveitis Overview
What are the key features of uveitis? Here are four important points to understand about this condition:
- Uveitis is inflammation inside the eye: Uveitis is characterized by inflammation within the eye, specifically in the uvea, which is the middle layer of the eye. This inflammation can damage various structures within the eye and affect its normal functioning.
- It can be caused by the immune system: Uveitis can occur when the immune system mistakenly attacks the healthy tissue of the eye, or when it fights off an eye infection. In some cases, the exact cause of uveitis remains unclear.
- Uveitis can affect one or both eyes: While uveitis can affect either eye, it is not uncommon for it to occur in both eyes simultaneously or at different times. It is essential to seek medical attention if you experience any symptoms of uveitis in either eye.
- Untreated uveitis can lead to vision loss: If left untreated, uveitis can cause permanent damage to the eye and lead to vision loss. It is crucial to seek prompt medical attention to prevent further complications and preserve your vision.
Understanding these key features of uveitis can help you recognize the symptoms and seek appropriate treatment to protect your eye health.
The Uvea
The uvea consists of three main components: the iris, ciliary body, and choroid. The iris is the colored part of the eye, located inside the front of the eye. It controls the amount of light that enters the eye by adjusting the size of the pupil. The ciliary body, located behind the iris, plays a role in helping the lens focus. It produces the fluid that fills the front part of the eye and nourishes the cornea and lens. The choroid is a layer of blood vessels between the retina and sclera. It supplies oxygen and nutrients to the retina and helps remove waste products. These three components of the uvea are crucial for the normal functioning of the eye. Any inflammation or damage to the uvea can lead to uveitis, a condition characterized by redness, pain, and vision problems. Understanding the role of the uvea can help in the diagnosis and treatment of uveitis.
Types of Uveitis
Uveitis can manifest in different forms depending on the specific part of the eye that is affected. Here are the different types of uveitis:
- Anterior uveitis: This type affects the iris at the front of the eye. It is the most common form of uveitis and can cause symptoms such as eye redness, pain, and light sensitivity.
- Intermediate uveitis: This type affects the ciliary body and vitreous, which is the gel-like substance filling the back of the eye. Symptoms may include blurred vision, floaters, and eye pain.
- Posterior uveitis: This type affects the retina and choroid at the back of the eye. It can cause symptoms such as decreased vision, floaters, and eye pain.
- Panuveitis: This type affects all parts of the uvea, including the iris, ciliary body, and choroid. It can cause a combination of symptoms from anterior, intermediate, and posterior uveitis.
Each type of uveitis has different symptoms and severity. It is important to seek medical attention if you experience any symptoms of uveitis, as untreated uveitis can lead to vision loss. Your eye doctor can provide a proper diagnosis and recommend appropriate treatment options.
Uveitis Risk Factors
If you have a family history of uveitis, you may be at an increased risk for developing this inflammatory condition that affects the eyes. While uveitis can affect anyone, certain risk factors can make some individuals more susceptible. Here are some key risk factors for uveitis:
| Risk Factors |
|---|
| Family history of uveitis |
| Age (more common in people aged 20 to 60) |
| Smoking cigarettes |
| Certain infections, autoimmune diseases, and cancers |
Having a family history of uveitis can increase your susceptibility to developing the condition. Additionally, uveitis is more commonly seen in individuals between the ages of 20 and 60. Smoking cigarettes has also been associated with a higher risk of uveitis. Certain infections, autoimmune diseases, and cancers can also increase the likelihood of developing uveitis.
It is important to note that having these risk factors does not necessarily mean that you will develop uveitis. However, being aware of these factors can help you take proactive steps to protect your eye health. Regular eye exams can help detect uveitis early, allowing for timely treatment and management. If you have any concerns or a family history of uveitis, it is recommended to consult with an eye care professional.
Anatomy of the Eye With Uvea
To understand the anatomy of the eye with uvea, you can start by examining the three main components: the iris, ciliary body, and choroid.
- Iris: The iris is the colored part of the eye located inside the front of the eye. It controls the amount of light that enters the eye by adjusting the size of the pupil.
- Ciliary Body: The ciliary body is situated behind the iris. It plays a crucial role in helping the lens of the eye focus on objects at different distances. It also produces the aqueous humor, a fluid that nourishes the eye.
- Choroid: The choroid is a layer of blood vessels located between the retina and the sclera (the white outer part of the eye). It supplies oxygen and nutrients to the retina and helps regulate its temperature.
- Retina: The retina lines the inside of the back of the eye and contains specialized cells called photoreceptors that detect light and send signals to the brain, allowing us to see.
Understanding the anatomy of the eye with uvea is important in comprehending how uveitis, inflammation of the uvea, can impact vision and overall eye health. The intricate interplay between the iris, ciliary body, choroid, and retina is essential for maintaining optimal visual function.
Causes of Uveitis
Understanding the causes of uveitis can help shed light on the factors that contribute to inflammation inside the eye. In about half of cases, the exact cause of uveitis is unclear. However, it is believed to be an autoimmune disease, where the immune system mistakenly attacks the healthy tissue of the eye. Other possible causes include infections, medication side effects, eye injury or surgery, and rarely, eye cancer. Certain autoimmune or inflammatory disorders affecting other parts of the body can also lead to uveitis. Additionally, changes in certain genes and smoking cigarettes have been associated with an increased risk of developing uveitis. It’s important to note that approximately one in three uveitis cases have no known cause. Identifying the underlying cause of uveitis is crucial for effective treatment and management of the condition. If you experience symptoms of uveitis, it is important to seek medical attention to determine the cause and receive appropriate treatment.
Treatment and Complications of Uveitis
Seeking prompt medical attention is crucial for the treatment and management of uveitis, as well as to minimize potential complications associated with the condition. Here are some important aspects of uveitis treatment and possible complications to be aware of:
- Treatment options: The appropriate treatment for uveitis depends on the type and severity of the condition. It may include medications such as antibiotics, antivirals, antifungals, eye drops, steroidal anti-inflammatories, and immunosuppressants. The choice of treatment aims to reduce inflammation, control pain, and prevent further damage to the eye.
- Duration of treatment: Uveitis treatment can vary in length. Some forms of uveitis may resolve within a few weeks, while others may require long-term or even lifelong treatment. It is important to follow the prescribed treatment plan and attend regular follow-up appointments to monitor progress.
- Recurrence: Uveitis can sometimes recur even after successful treatment. In such cases, additional treatment may be necessary. It is important to communicate any changes in symptoms to your healthcare provider to ensure appropriate management.
- Complications: If left untreated or poorly managed, uveitis can lead to complications that can affect vision. These can include ocular hypertension (increased eye pressure), glaucoma, cataracts, cystoid macular edema (swelling in the central part of the retina), and damage to the vitreous gel substance. Regular monitoring of the condition and timely intervention can help minimize the risk of complications and preserve vision.