Have you ever felt like one side of your face was playing a different tune, like a symphony out of harmony? It could be a sign of Horner’s Syndrome, a condition that disrupts the normal functioning of your eye and the surrounding tissues. From drooping eyelids to constricted pupils, these symptoms can be a cause for concern. But what exactly causes Horner’s Syndrome and how can it be treated? Let’s dive into the details and uncover the answers together.
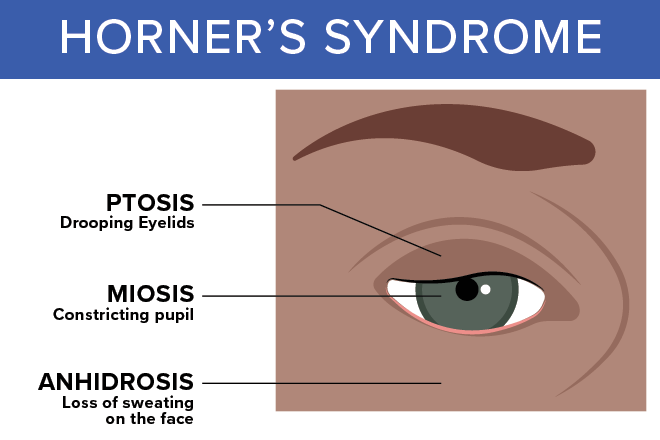
Drooping Eyelid (Ptosis)
Drooping eyelid, also known as ptosis, is a medical condition characterized by the sagging of the upper eyelid. In Horner’s Syndrome, ptosis is one of the key symptoms. The drooping eyelid occurs on the affected side of the face due to a disruption in the nerve pathway from the brain to the head and neck. It can be caused by various underlying conditions such as a stroke, tumor, or spinal cord injury.
When it comes to treatment options for drooping eyelid in Horner’s Syndrome, there are a few approaches available. One option is cosmetic surgery, which can help correct the appearance of the eyelid. Another treatment option is the use of eyedrops, which can provide temporary relief by helping to elevate the eyelid. It’s important to note that these treatments address the ptosis itself and not the underlying cause of Horner’s Syndrome.
In terms of long-term management, the focus is on treating the underlying cause of Horner’s Syndrome. By addressing the root cause, it may be possible to restore nerve function and alleviate the drooping eyelid. Regular monitoring and follow-up with healthcare providers is essential to track progress and manage any complications that may arise. Overall, the prognosis for drooping eyelid in Horner’s Syndrome depends on the success of treating the underlying cause and the extent of nerve damage.
Constricted Pupil (Miosis)
One of the key symptoms of Horner’s Syndrome is the presence of a constricted pupil, also known as miosis. When you have Horner’s Syndrome, the pupil in the affected eye is smaller than the pupil in the unaffected eye. This occurs because the disruption of sympathetic nerve pathways leads to a decrease in the size of the pupil.
To effectively manage Horner’s Syndrome, it is important to address the underlying cause. Treatment options depend on the specific condition causing the syndrome. Surgical intervention may be necessary if a tumor or other treatable cause is identified. Medications may also be prescribed to manage symptoms or target the underlying condition.
Diagnostic tests play a crucial role in identifying the underlying cause of Horner’s Syndrome. Imaging tests such as chest X-rays, MRI, CT scans, or ultrasounds may be ordered to detect any structural abnormalities or tumors. These tests help healthcare providers determine the appropriate management strategies for each individual.
The prognosis of Horner’s Syndrome depends on the underlying condition and the extent of nerve damage. In some cases, Horner’s Syndrome may resolve on its own. Complications can include vision problems, facial asymmetry, or functional limitations. Regular monitoring and follow-up with healthcare providers are essential to ensure proper management and prevent complications.
Decreased Sweating or Anhidrosis
Patients with Horner’s Syndrome may experience a decrease in sweating, a condition known as anhidrosis, on the affected side of their face. Anhidrosis is one of the key symptoms of Horner’s Syndrome and can occur due to disruption of the sympathetic nerve pathway. The underlying causes of decreased sweating in Horner’s Syndrome can vary, ranging from blockage or damage to sympathetic nerves to conditions such as middle ear infection or carotid artery dissection. Diagnosis of anhidrosis usually involves a physical examination and detailed questioning about symptoms and medical history. Treatment options for anhidrosis in Horner’s Syndrome focus on addressing the underlying cause. Surgical intervention may be necessary if the cause is known and treatable, such as a tumor. Medications may be prescribed to manage symptoms or address specific causes. Additionally, managing other symptoms such as drooping eyelid (ptosis) is an important aspect of Horner’s Syndrome treatment. Regular monitoring and follow-up with healthcare providers is essential to ensure appropriate management of anhidrosis and other associated symptoms. It is important to note that anhidrosis, along with other symptoms like miosis (constricted pupil), can have implications for the overall prognosis and management of Horner’s Syndrome. Redness or flushing on the affected side may also be present and should be considered in the evaluation and management of the condition.
Redness or Flushing of the Affected Side
The presence of redness or flushing on the affected side of the face is another notable symptom that can be observed in individuals with Horner’s Syndrome. This redness is caused by the disruption of sympathetic nerves that control blood flow to the face. Here are some key points to help you understand the causes, evaluation, management, and impact of redness in Horner’s Syndrome:
Causes and mechanisms of redness in Horner’s Syndrome:
- Redness occurs due to the interruption of sympathetic nerve fibers that regulate blood vessel constriction in the face.
- The disruption of these nerves leads to increased blood flow and dilation of blood vessels, resulting in redness or flushing.
Clinical evaluation and diagnostic tests for redness in Horner’s Syndrome:
- A thorough physical examination is crucial to assess the presence and extent of redness.
- Additional tests, such as imaging studies (MRI, CT scan) and ophthalmic evaluations, may be performed to identify the underlying cause and confirm the diagnosis of Horner’s Syndrome.
Management and treatment options for redness in Horner’s Syndrome:
- The primary focus of treatment is addressing the underlying cause of Horner’s Syndrome.
- Treatment may involve medications, surgical interventions, or other therapeutic approaches depending on the specific cause identified.
Redness in Horner’s Syndrome: impact on quality of life and daily activities:
- The presence of redness can be aesthetically bothersome to individuals with Horner’s Syndrome, potentially impacting their self-esteem and quality of life.
- Redness may also affect daily activities, particularly in social and professional settings.
Research advancements and future directions in understanding redness in Horner’s Syndrome:
- Ongoing research is focused on further understanding the mechanisms of redness in Horner’s Syndrome and developing targeted interventions.
- Advances in imaging techniques and molecular studies are expected to contribute to a deeper understanding of the condition and potential treatment options.
Sinking of the Eyeball Into the Face
When Horner’s Syndrome is present, one noticeable symptom is the sinking of the eyeball into the face. This sinking of the eyeball, also known as enophthalmos, occurs due to the disruption of sympathetic nerve pathways that control the muscles and tissues around the eye.
Causes of eyeball sinking can vary and may include trauma to the eye or face, tumors, or inflammation in the surrounding structures. The impact of eyeball sinking on vision can be significant, as it can result in a decrease in visual acuity and a narrowing of the visual field.
Surgical options are available for correcting eyeball sinking, depending on the underlying cause. These may include reconstructive surgery to restore the position of the eyeball and improve its appearance.
The psychological effects of eyeball sinking should not be overlooked. Individuals may experience self-consciousness, depression, or anxiety due to the changes in their appearance. It is important to address these psychological effects and provide support and counseling as needed.
In addition to surgical interventions and psychological support, lifestyle modifications can also play a role in managing eyeball sinking. These may include wearing protective eyewear, practicing good eye hygiene, and maintaining a healthy lifestyle to promote overall eye health.
Different Sizes of Pupils (Anisocoria)
Anisocoria, or different sizes of pupils, is a common symptom associated with Horner’s Syndrome. When one pupil is smaller than the other, it can indicate a disruption in the sympathetic nerve pathway. Here is some important information about anisocoria in relation to Horner’s Syndrome:
Causes of anisocoria:
- Interruption in nerve fibers from the hypothalamus
- Injury to the carotid artery or brachial plexus
- Migraine or cluster headaches
- Stroke, tumor, or damage to the brainstem
Nerve fiber location and associated symptoms:
- First-order (central) nerve pathway: may cause sinking of the eyeball into the face
- Second-order (preganglionic) nerve pathway: may result in ptosis (drooping eyelid)
- Third-order (postganglionic) nerve pathway: can lead to anhidrosis (decreased sweating on the affected side of the face)
Treatment options for anhidrosis:
- Treatment focuses on addressing the underlying cause of Horner’s Syndrome
- Medications may be prescribed to manage symptoms or treat specific causes
- Physical therapy or rehabilitation may be recommended to improve function
Ptosis management:
- Ptosis, or drooping eyelid, can be corrected with cosmetic surgery or the use of eyedrops
Evaluation of sinking eyeball:
- An eye exam may be conducted to observe changes in pupil and eyelid
- Additional tests such as imaging tests (MRI, CT scan) may be ordered to identify any structural abnormalities or tumors
Understanding the causes, associated symptoms, and treatment options for anisocoria in Horner’s Syndrome is crucial for proper management and care. Seek medical attention for an accurate diagnosis and to determine the best course of treatment.
Additional Symptoms Depending on Affected Nerve Fiber Location
To further understand the impact of Horner’s Syndrome on the affected individual, it is important to explore the additional symptoms that can manifest depending on the location of the affected nerve fiber. The nerve fiber location plays a crucial role in determining the specific symptoms experienced by the individual. For example, if the first-order nerve fibers are affected, you may experience facial coloration changes on the affected side of the face. This can manifest as redness or flushing of the skin. On the other hand, if the second-order nerve fibers are affected, you may notice a lighter iris color in the affected eye. This change in iris color is known as heterochromia. Lastly, if the third-order nerve fibers are affected, you may experience sinking of the eyeball into the face, a condition known as enophthalmos. It is important to note that these additional symptoms depend on the location of the affected nerve fiber and can vary from person to person. Additionally, the underlying conditions causing Horner’s Syndrome can also contribute to the manifestation of these additional symptoms. Therefore, it is crucial to consult with a healthcare professional for a comprehensive evaluation and appropriate management of Horner’s Syndrome.